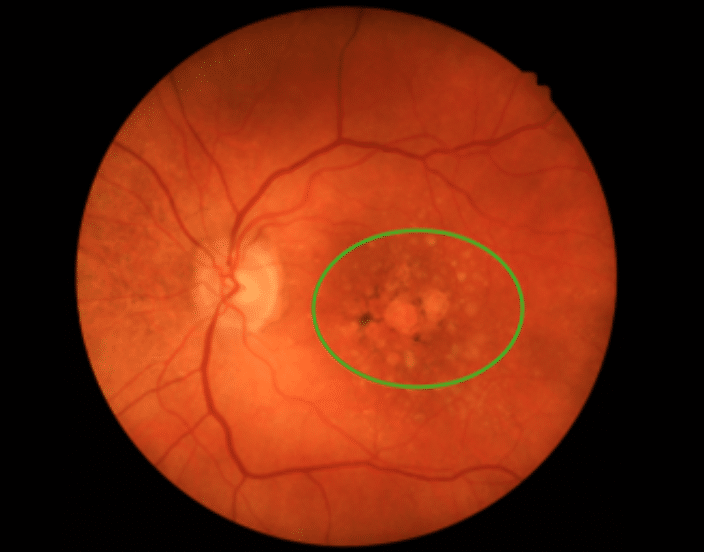
Introduction To Glaucoma
Why Do People Get Glaucoma
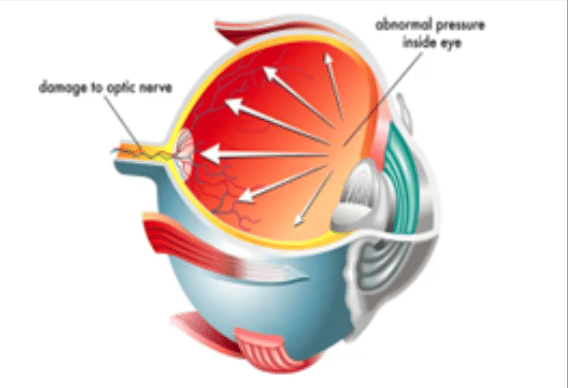
Glaucoma, often referred to as the “silent thief of sight”, can progress without noticeable symptoms until significant vision loss has occurred, making it the leading cause of blindness worldwide.
Understanding glaucoma is crucial as it silently progresses, often leading to significant and irreversible vision loss. If glaucoma goes undiagnosed, it can gradually and irrevocably deteriorate vision.