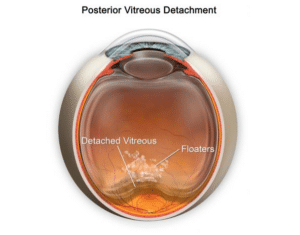
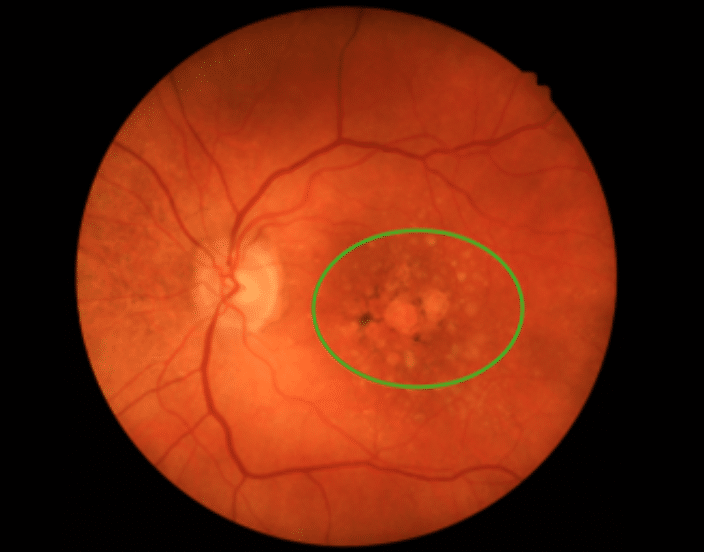
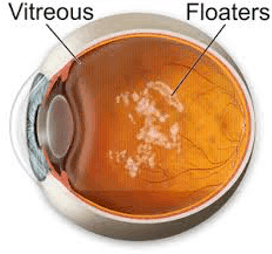
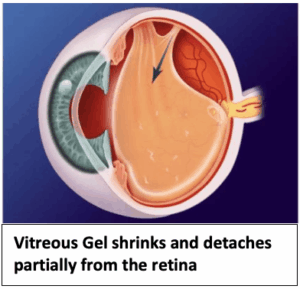
Floaters, those intriguing specks or cobweb-like shadows drifting across one’s vision, signify natural changes within the vitreous gel of the eye. Far from being a mere distraction, these floaters serve as reminders of the intricate and marvellous workings of the human eye.
Often appearing as dots, lines, or ambiguous shapes, these visual phenomena can arise suddenly, though they might have been building up subtly over time. Their presence in our field of vision, while typically benign, commands our awareness of any sudden onsets or dramatic increases in their number.
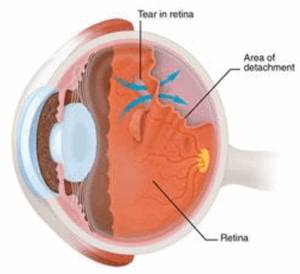
Moreover, floaters frequently accompany flashes, bursts of light seen even in darkness. Such flashes, stemming from mechanical pulls on the retina, can heighten one’s intuition that something may warrant medical investigation.
It’s vital to bear in mind that floaters naturally evolve with age, predominantly benign and stable in nature, requiring no treatment unless dramatic changes surface. Awareness and observation become key, as monitoring one’s symptoms can vastly aid in distinguishing between harmless floaters and more significant retinal issues.
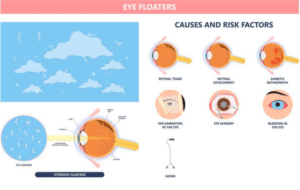
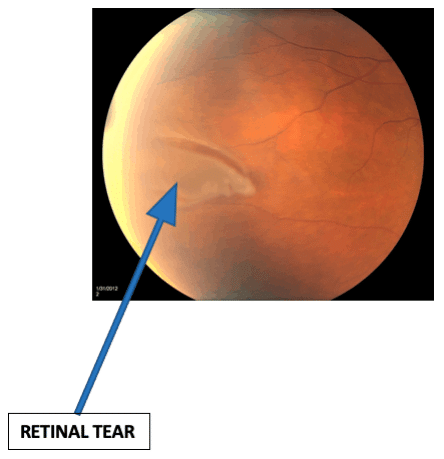
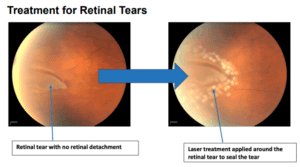
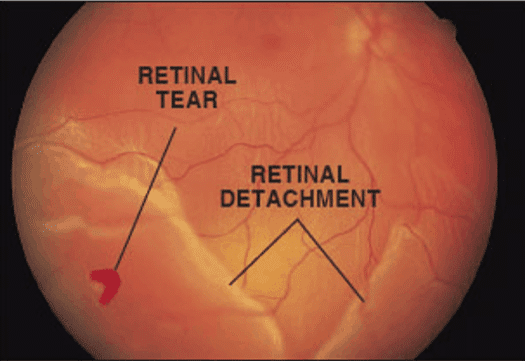
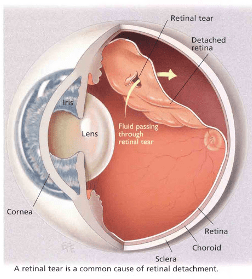
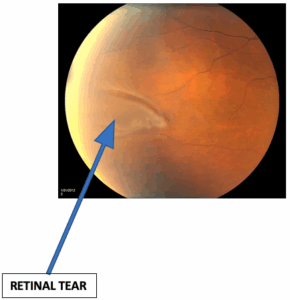
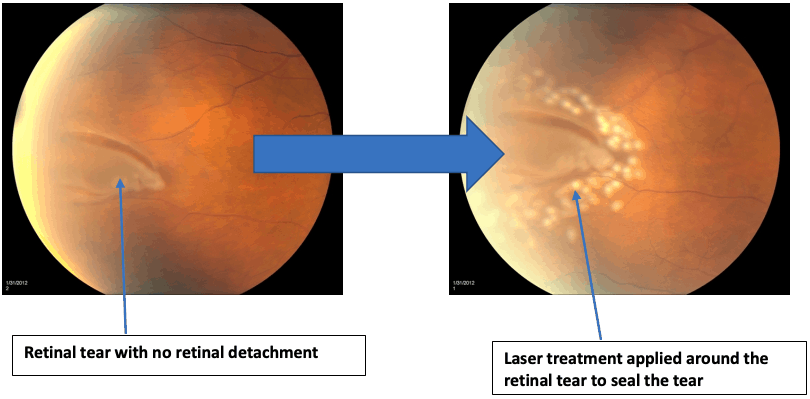
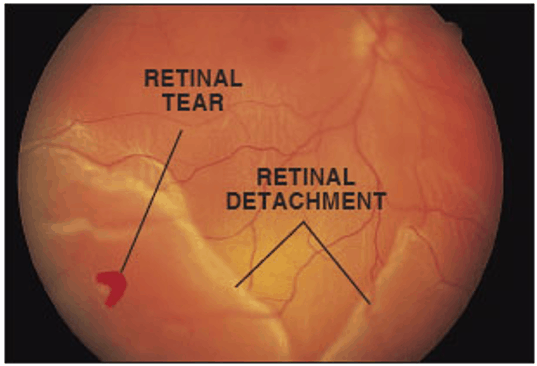
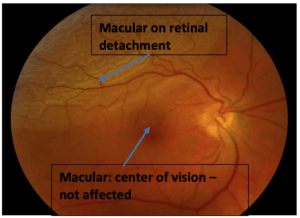
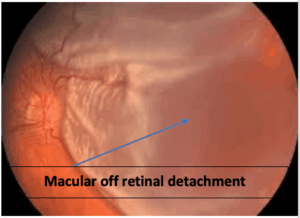
When new floaters emerge or an unexpected ‘shower’ of these spots occurs, it may be indicative of more serious retinal conditions such as a tear or detachment that requires urgent attention. Professional evaluation ensures peace of mind and can prevent potential complications from escalating.
Ultimately, the dance of floaters across one’s vision is a call to remain vigilant regarding eye health. By recognising these symptoms, individuals empower themselves, fortifying their commitment to an enduring and flourishing vision.